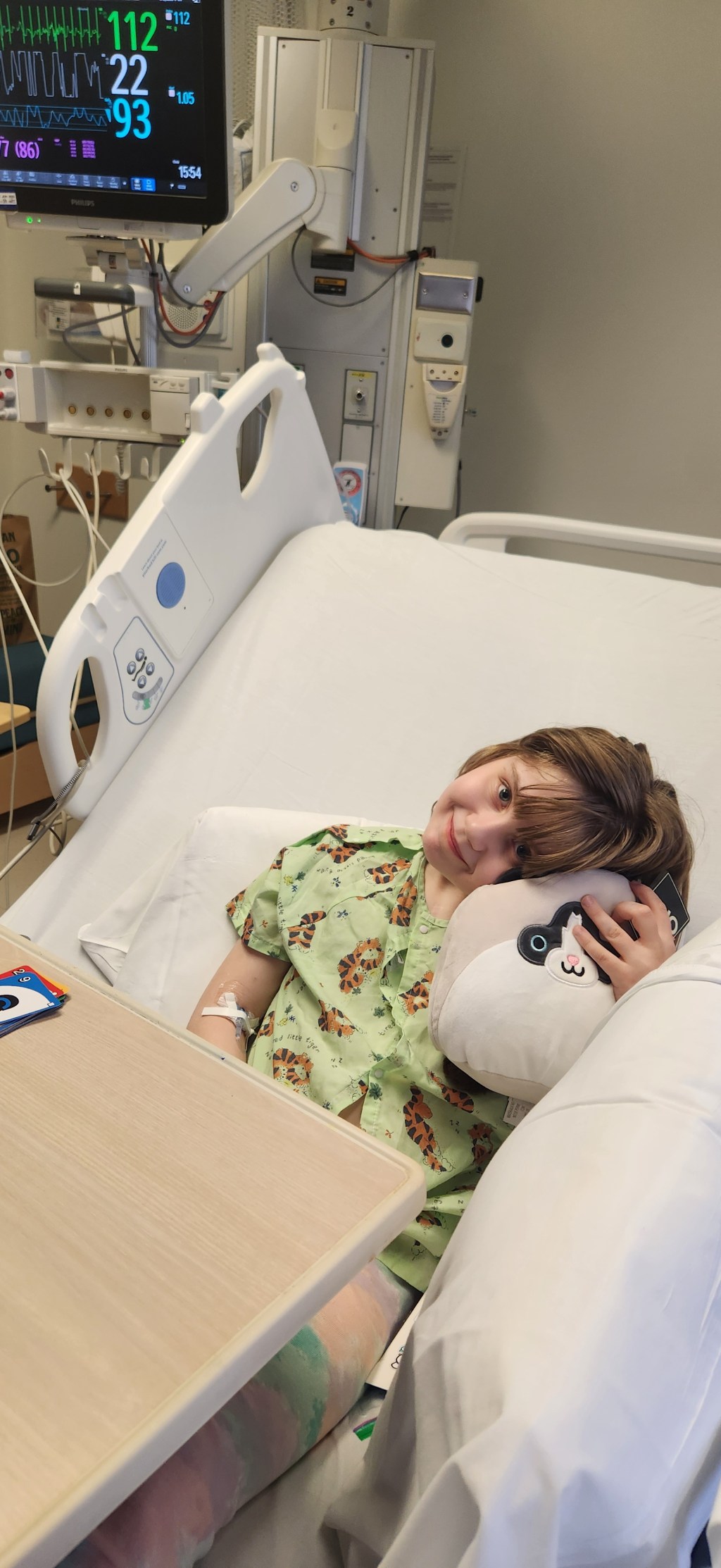
It’s been a really rough few months for Katja. She started with a minor cold in late Nov that progressed to pneumonia within 2 weeks. Since then, she’s had multiple antibiotics, steroids and medication changes including significantly reducing her immunosuppressants.
However, her pneumonia continues to return. This is what lead to her being hospitalized last month. We’ve noticed an increased sensitivity to getting sick and activating her asthma/airway inflammation.
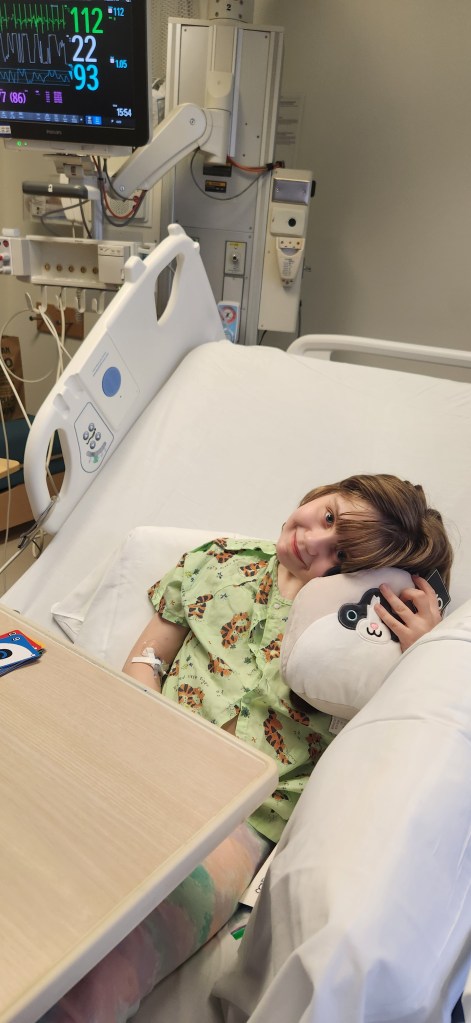
This week Katja was doing well, within 24hrs she became pale, sweaty and extremely tired. She didn’t have a fever and had been perfectly fine just an hour earlier. I found her fast asleep on the couch. I decided to check her oxygen saturation and to my shock it was 85. She was at 97 just that morning.
We immediately got her set up on her home oxygen and paged her teams. She improved and stabilized overnight on oxygen but the following morning she was still pale and tired.
We took her to the Pediatrician’s urgent care and an X-ray confirmed that her pneumonia had returned. She was sent to Seattle Children’s ER and admitted yesterday. During admissions we’ve discovered that Katja has severe Neutropenia.
What is Neutropenia?
– is a blood disorder characterized by an abnormally low level of neutrophils, a type of white blood cell essential for fighting bacterial infections —usually resulting from decreased production in the bone marrow.
The medications used to protect Katja from viral infections and from rejection are affecting her neutrophils and her bone marrow production. To top it off, multiple pneumonias plus lots of steroids have significantly reduced these numbers further.
She is essentially fighting a bacterial war inside her body with no ammunition. This explains why she’s getting so many pneumonia infections.
Her teams are working hard together on a solution. There is a very delicate balance here. If they reduce immunosuppressants to much or try to artificially stimulate bone marrow production (G-CSF) is could trigger her body to reject her heart pieces. But if we do nothing, we risk a minor cold causing significant complications.
We are starting with the easiest fix, removing her anti viral meds and hoping her body responds. If it doesn’t we may need to temporarily stop 1 of her 2 immunosuppressants to give her immune system a chance to fight again.
After everything Katja has been through, this is obviously not how we hoped her recovery would go. These are some of the risks we took when picking a PHT. However, we wouldn’t change that choice. Her heart is handling all of this wonderfully and without that PHT I don’t think she’d have survived pneumonia 3 times in 6 weeks (and she is prone to pneumonia even when not on transplant meds).
She is such a strong, resilient little girl and she’s been through so so much in her short 10 years on this earth. I would trade places with her in a heartbeat if I could. I don’t know what lessons the universe is teaching Katja but I have high hopes for extraordinary things from this extremely special girl.
As always, she remains #KatjaStrong